Call Us Today!
(703) 669-8688
New Patients
(703) 202-1740

At the office of Village Dental of Leesburg, our priority is to preserve natural teeth whenever possible. Still, there are circumstances where extracting a tooth is the most responsible choice to protect a patient’s long-term oral health and comfort. We approach every case with careful evaluation, clear explanations, and a focus on minimizing pain and preserving function.
To decide whether an extraction is necessary, we consider factors like the extent of decay or damage, the health of surrounding gums and bone, infection risk, and how a problematic tooth affects nearby teeth or orthodontic plans. Our team will review your full medical and dental history, examine the area thoroughly, and use diagnostic imaging when needed to make an informed recommendation.
When an extraction is advised, we take time to explain why the procedure is recommended, what to expect during the visit, and the potential options for replacing the tooth afterward. Our goal is to give patients enough information to feel confident about the treatment plan and the next steps for restoring comfort and function.
Primary (baby) teeth that won’t shed naturally
Sometimes a baby tooth remains firmly in place because its root didn’t resorb, or the tooth has become fused to the bone. When that happens, the retained tooth can block the eruption of the permanent tooth, interfere with proper alignment, and cause orthodontic complications. Removing an over-retained tooth is often the most direct way to allow normal development.
Permanents with extensive decay beyond restoration
When decay has destroyed most of a tooth's structure or reached the root system, there may not be enough healthy material left to support a filling or crown. In those cases, extraction prevents ongoing infection and pain and protects adjacent teeth and tissues.
Teeth fractured below the gum line or with compromised roots
A severe fracture that extends into the root or splits a tooth can make repair impractical or impossible. If a tooth cannot be predictably restored to function, removing it may be the safest option.
Advanced periodontal disease
Periodontal disease can erode the bone and soft tissues that support teeth. When a tooth becomes loose or the supporting structures are significantly diminished, extraction may be necessary to stop the spread of disease and stabilize surrounding teeth.
Impacted or problematic wisdom teeth
Third molars often don’t have enough room to erupt properly, which can lead to partial eruptions, decay, or damage to neighboring teeth. Removing impacted wisdom teeth can prevent recurrent pain, infections, and crowding.
Extractions as part of orthodontic planning
When a jaw is too small to accommodate all of the permanent teeth, selective removal may be part of an orthodontic strategy to create space, improve alignment, and establish a stable bite.
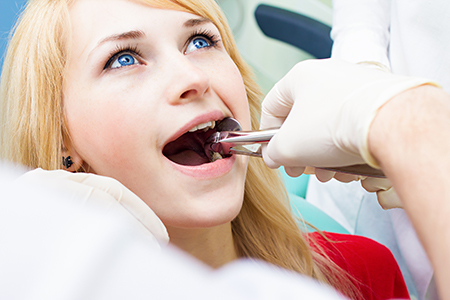
Before any extraction, we'll take time to review your medical history, current medications, and any conditions that could affect treatment or healing. Clear communication about allergies, blood thinners, recent illnesses, and other medical matters helps us tailor care and take appropriate precautions for a safe outcome.
To plan the procedure precisely, we use digital radiographs when indicated. These images show the shape and position of the roots, the relationship to surrounding bone, and whether the tooth is impacted or has unusual anatomy. Imaging lets us anticipate potential challenges and determine whether a simple or surgical approach is needed.
Local anesthesia is used to numb the area so patients remain comfortable during the extraction. For those who experience anxiety or require more extensive sedation, we offer options to help patients relax; we’ll discuss these choices and any pre-procedure steps well in advance so you can prepare.
Simple extractions are performed on teeth that are fully visible in the mouth and have a straightforward root structure. After numbing the area, the dentist gently loosens the tooth and removes it with forceps. The process is typically quick and designed to minimize trauma to surrounding tissues.
Surgical extractions are required when a tooth is broken at the gum line, impacted, ankylosed, or has complex root anatomy. These procedures can involve a small incision and the removal of a bit of bone to access the tooth. When a case is beyond routine scope—such as with difficult impactions—we coordinate care with an oral and maxillofacial surgeon to ensure the best surgical outcome for the patient.
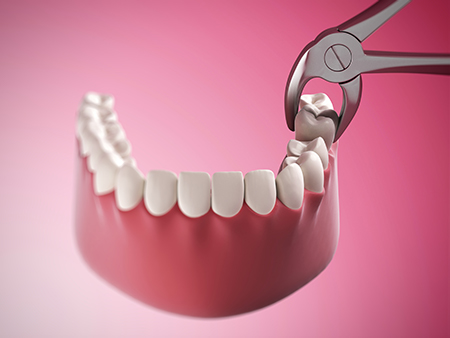
Every patient’s recovery timeline is different, but most people can expect gradual improvement over several days. Our team provides clear, written aftercare instructions tailored to the type of extraction performed. Following those guidelines helps reduce discomfort, minimize swelling, and lower the risk of complications like infection or dry socket.
During the first 24–48 hours, it’s common to experience mild bleeding, swelling, and soreness. Simple strategies such as careful rest, short intervals of cold application, and avoiding actions that disturb the clot (like vigorous rinsing or using a straw) promote healing. If sutures were placed, we’ll let you know whether they are dissolvable or if a follow-up visit is needed for removal.
We advise patients to bring a list of questions to their post-procedure appointment and to contact the office if unusual pain, prolonged bleeding, fever, or other concerning symptoms occur. Timely communication ensures any issues are addressed quickly and safely.
Control bleeding with gauze
Bite gently on the provided gauze for the time recommended by your clinician. If bleeding persists, replacing the gauze and maintaining steady pressure typically helps. Persistent heavy bleeding should be reported to our office.
Protect numb tissues
Until the anesthetic fully wears off, avoid chewing or touching the area to prevent accidental biting of lips, tongue, or cheeks.
Follow medication guidance
Take any prescribed antibiotics or pain medications exactly as directed. Over-the-counter non-aspirin pain relievers can also help manage discomfort unless otherwise advised by your provider.
Allow the clot to form
Avoid rinsing vigorously, spitting forcefully, and using straws for several days. These actions can dislodge the clot and delay healing.
Reduce swelling with ice
Apply a cold pack to the outside of the cheek in short intervals on the day of the procedure to manage swelling.
Skip tobacco
Smoking impairs healing and increases the risk of complications. Avoid tobacco products for at least one week after surgery.
Choose soft foods
Stick to cool or lukewarm soft foods for a few days. Avoid hot, crunchy, or spicy items until healing is well underway.
Maintain gentle oral hygiene
Keep your mouth clean by brushing other teeth carefully and, when appropriate, rinsing gently with a mild saline solution after the first 24 hours.
Attend follow-up appointments
If a follow-up visit is scheduled—for suture checks, complex cases, or signs of infection—attend as instructed so we can confirm healthy healing.
Contact our team if you notice increased pain, swelling that worsens after a few days, persistent bleeding, fever, or any other symptom that seems unusual. Prompt attention helps prevent minor problems from becoming more serious.
Removing a tooth often raises questions about how to restore chewing ability and the look of the smile. We will review replacement options suited to your needs, oral health, and long-term goals. Choices commonly include removable dentures, fixed bridges, and dental implants. Each approach has advantages and considerations that we’ll review so you can make an informed decision.
Dental implants recreate a tooth root with a titanium post and can support a crown, bridge, or denture. They are designed to integrate with the jawbone and can offer a stable, long-term solution for many patients. Fixed bridges replace one or more missing teeth by anchoring to adjacent teeth, while partial or complete dentures provide removable alternatives for replacing multiple teeth.
We’ll discuss the timeline for replacement—such as immediate versus delayed options—and how bone health, gum condition, and overall medical considerations influence the recommended approach. When additional procedures are needed, such as bone grafting or periodontal treatment, we’ll explain the sequence of care and coordinate referrals when appropriate.
Preparing for an extraction includes practical steps and clear communication. Ask about what type of anesthesia will be used, whether you’ll need a companion to drive you home, and any medication instructions to follow beforehand. If you take blood thinners or have medical conditions such as diabetes or heart disease, inform us so we can coordinate with your physician when necessary.
On the day of the procedure, follow pre-operative instructions closely—these may include fasting if you will receive sedation. After the extraction, keep the lines of communication open: report unexpected symptoms promptly and attend scheduled follow-up visits so healing can be monitored and any restorative planning can proceed on schedule.
Our team is committed to answering questions and helping patients feel prepared. If you’d like to learn more about extraction care or restorative options, please contact us for additional information and to arrange a consultation.
Extractions are recommended when a tooth cannot be saved by restorative or periodontal treatment and poses a risk to overall oral health. Common reasons include extensive decay that compromises the tooth structure, severe fracture below the gum line, advanced periodontal disease with significant bone loss, or teeth that obstruct the eruption of others. Diagnostic imaging and a careful clinical exam help determine whether removal is the safest option.
Primary (baby) teeth that fail to shed and impacted third molars are other frequent indications for extraction, especially when they affect alignment or cause recurrent infection. We also consider how a problematic tooth interacts with orthodontic plans or prosthetic needs before recommending removal. The decision is individualized to balance preserving natural teeth with preventing future complications.
Most patients experience minimal pain during an extraction because the area is numbed with local anesthesia and, when appropriate, sedation options are available to help manage discomfort and anxiety. During simple extractions the procedure is typically quick and sensations are limited to pressure rather than sharp pain, while surgical extractions may involve more aftercare but are performed under adequate anesthesia. Your dental team will review anesthesia choices and any pre-procedure instructions to optimize comfort.
After the procedure, some soreness, swelling, and mild bleeding are common as tissues begin to heal, and these symptoms are usually controlled with prescribed or recommended analgesics and home care measures. Following post-operative instructions reduces the risk of complications and speeds recovery, and the office should be contacted if pain worsens or does not improve. At Village Dental of Leesburg we emphasize clear communication so patients know what to expect and how to manage discomfort safely.
A simple extraction is performed on a tooth that is fully visible in the mouth and has a straightforward root structure; it is removed with forceps after local anesthesia. Surgical extractions are required when a tooth is broken at the gum line, impacted, ankylosed, or has unusual root anatomy, and these procedures may involve small incisions, removal of a bit of bone, or sectioning the tooth for safer removal. The choice between simple and surgical approaches is based on imaging and clinical evaluation.
Surgical cases can be managed in the dental office when appropriate, but complex impactions or medically complicated patients may be referred to an oral and maxillofacial surgeon for specialized care. Your clinician will explain the recommended approach, the reasons for referral if needed, and the expected aftercare for a surgical procedure. Anticipating potential challenges through diagnostic imaging helps ensure a safe, predictable outcome.
Preparing for an extraction begins with a thorough review of your medical and dental history, including current medications, allergies, and any chronic conditions such as diabetes or heart disease. If you take blood thinners or other medications that affect bleeding or healing, inform the office well in advance so the team can coordinate care with your physician if necessary. Follow any pre-procedure instructions regarding fasting when sedation is planned and arrange for a companion to drive you home if you will receive sedative medications.
On the day of the appointment wear comfortable clothing and avoid heavy makeup or jewelry that might interfere with monitoring if sedation is used. Bring a list of questions about anesthesia, post-operative care, and replacement options so you feel prepared for the next steps. Clear communication about expectations and any special needs helps the team tailor the experience for a safe and comfortable procedure.
Initial healing typically progresses over several days, with noticeable improvement each day as swelling and discomfort diminish; most patients return to normal activities within a few days depending on the complexity of the extraction. In the first 24–48 hours it is normal to have mild bleeding, swelling, and soreness, and following instructions such as gentle rest, cold applications, and avoiding actions that disturb the clot will support healing. Maintain gentle oral hygiene around the surgical site and follow guidance on diet, activity, and medications provided by your clinician.
Sutures, if placed, may be dissolvable or require removal at a follow-up visit, and your dental team will advise on the timeline for suture care and any required appointments. Avoid smoking and tobacco for at least a week, as these delay healing and increase the risk of complications like dry socket. If symptoms such as increasing pain, heavy bleeding, fever, or persistent swelling occur, contact the office promptly for evaluation.
While most extractions heal without issue, certain symptoms warrant prompt attention because they may indicate complications such as infection, alveolar osteitis (dry socket), or prolonged bleeding. Warning signs include increasing or severe pain beginning several days after the procedure, fever, persistent or heavy bleeding despite pressure, foul taste or odor, or swelling that worsens after the initial post-operative period. Any of these signs should prompt contact with the dental office so the team can evaluate and intervene as needed.
Dry socket typically presents as intense, localized pain a few days after extraction and may be accompanied by an empty-looking socket or exposed bone; treatment can alleviate symptoms and promote healing. Infections may require prescription antibiotics and targeted care, so timely communication prevents escalation. Keep scheduled follow-ups and report unexpected changes promptly to ensure safe recovery.
The timing for tooth replacement depends on several factors, including the condition of the surrounding bone and soft tissue, the presence of infection, and the chosen replacement method such as an implant, bridge, or denture. In some cases an immediate temporary restoration can be placed at the time of extraction, while other situations require a healing period to allow bone and gum tissues to stabilize before definitive treatment. Your clinician will assess bone volume, gum health, and overall treatment goals to recommend an appropriate timeline.
Dental implants often require several months of healing for the implant to integrate with the jawbone, and bone grafting may be necessary beforehand if significant bone loss is present. Fixed bridges and partial dentures have different sequencing and may involve preparing adjacent teeth or fabricating appliances after the extraction site has healed sufficiently. A coordinated plan helps restore function and appearance while preserving long-term oral health.
Not all wisdom teeth require removal; if third molars are fully erupted, healthy, properly aligned, and easy to clean, they may be monitored rather than extracted. Extractions are recommended when wisdom teeth are impacted, partially erupted and prone to decay, causing pain or infection, damaging adjacent teeth, or contributing to crowding. The decision is made after clinical examination and imaging that show how the third molars relate to surrounding structures.
For patients with impacted or problematic wisdom teeth we discuss the likely course, potential risks of leaving them in place, and the recommended timing for removal to reduce future complications. Younger patients often heal more quickly, which is one reason early evaluation is beneficial. Complex impactions may require surgical removal and, in selected cases, referral to an oral surgeon for specialized care.
We recognize that dental anxiety is common and offer several approaches to make the extraction experience more comfortable, including thorough explanations of the procedure, breathing and relaxation techniques, and pharmacologic options when appropriate. Local anesthesia is used as a standard to eliminate pain, and for patients with significant anxiety or extensive procedures we discuss conscious sedation or other controlled sedation modalities to help them relax. Prior to any sedative medication we review medical history and provide clear pre- and post-procedure instructions to ensure safety.
Staff members receive training in monitoring and supporting sedated patients, and we follow protocols for recovery and discharge, including requiring a responsible adult to drive you home when sedation is used. Open communication about fears and previous experiences allows the team to tailor care and provide a calming environment. If specialized anesthesia or hospital-based care is needed, the office will coordinate appropriate referrals to ensure patient comfort and safety.
Removing a tooth can influence bite dynamics and the position of adjacent teeth over time, particularly if the space is left unfilled; neighboring teeth may drift into the gap and opposing teeth can over-erupt, potentially altering chewing function and alignment. This is why replacement planning is an important part of extraction discussions and why clinicians evaluate the long-term functional and esthetic implications before recommending removal. The type of tooth, its role in the bite, and the patient’s overall dental health inform the recommended restorative approach.
Options such as dental implants, fixed bridges, or removable prostheses restore chewing ability and help preserve the position of adjacent teeth when appropriate. For patients undergoing orthodontic treatment, extractions may be planned strategically to improve alignment and occlusion rather than harming it. A coordinated plan between restorative and orthodontic specialists, when needed, supports predictable outcomes for function and aesthetics.
