Call Us Today!
(703) 669-8688
New Patients
(703) 202-1740
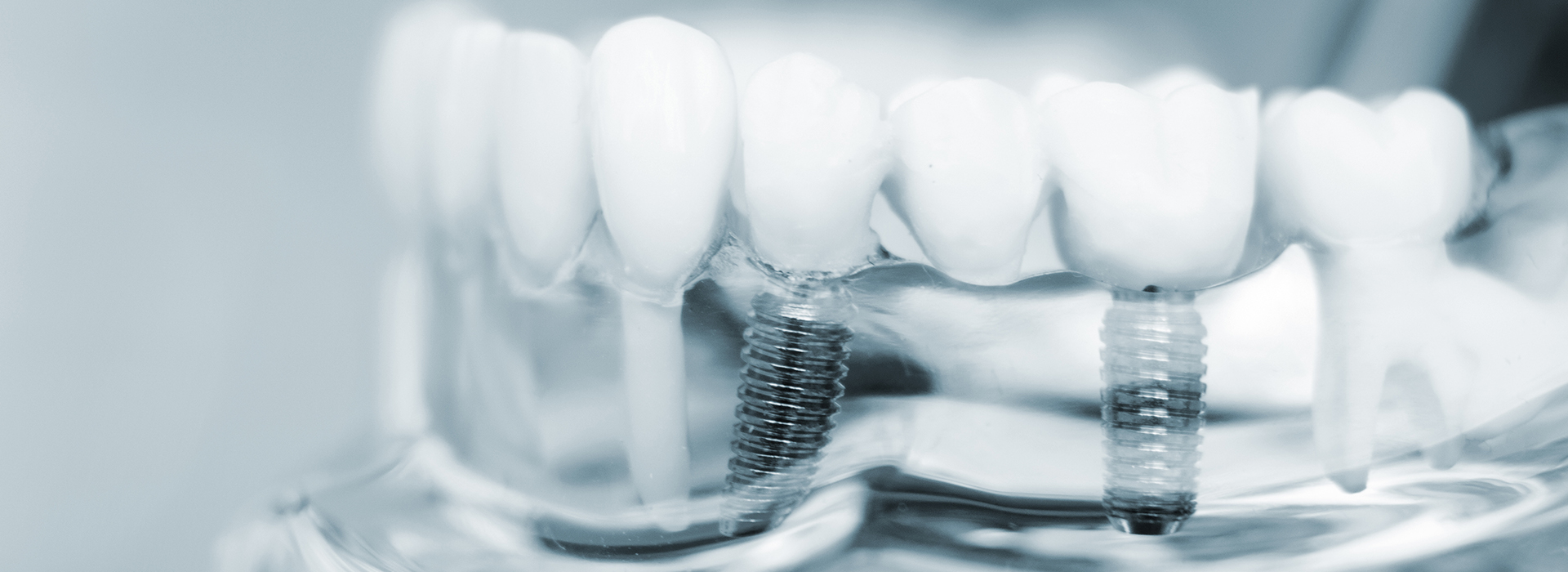
Missing teeth change more than just the way your smile looks — they alter how your mouth works and how your face ages. Teeth play an essential role in chewing, speaking, and supporting the soft tissues of the face. When a tooth is lost, the surrounding bone can begin to shrink and nearby teeth may shift to fill the gap, which can lead to bite problems, uneven wear, and added stress on remaining teeth.
Dental implants are designed to address those underlying issues by replacing not only the visible portion of a tooth but also its root-like function. By integrating with the jawbone, implants provide a stable foundation that helps preserve bone volume and maintain facial structure. That stability makes it easier to eat a wide variety of foods, speak clearly, and feel confident when you smile.
The team at Village Dental of Leesburg approaches tooth replacement with an eye toward both form and function. We focus on restoring a dependable bite and a natural appearance so that patients can enjoy durable results that blend seamlessly with their existing teeth.

Modern implant restorations are crafted to match the color, shape, and texture of natural teeth. Because each crown or prosthesis is custom-designed, implants can be nearly indistinguishable from surrounding teeth — even up close. The result is a smile that looks genuine and behaves like your original dentition when you chew, laugh, and speak.
Beyond appearance, implants restore function in a way removable prostheses often cannot. Fixed implant restorations are firmly anchored, eliminating common issues like slipping or clicking. That means increased confidence in social situations and fewer dietary limitations compared with traditional dentures.
When planning a restoration, we balance aesthetic goals with functional needs. Your restoration will be designed to harmonize with your bite, facial features, and personal preferences, producing an outcome that’s both practical and pleasing to the eye.
A dental implant is a small, biocompatible post — typically made from titanium or a titanium alloy — that is surgically placed into the jawbone where a tooth is missing. Over time, the bone forms a close bond with the implant in a process called osseointegration, creating a secure anchor for a crown, bridge, or denture.
Because implants mimic the role of natural tooth roots, they provide the mechanical support necessary for stable, long-lasting restorations. That root-like function also helps transmit chewing forces to the bone, which encourages healthy bone maintenance and prevents the gradual bone loss that follows tooth extraction.
Implants are versatile and can support single crowns, multi-unit bridges, or full-arch prostheses depending on the patient’s needs. Our treatment planning emphasizes precision — from 3D imaging and surgical guides to carefully designed final restorations — so each implant is placed and restored with predictable results.
Dental implants offer a range of benefits that can be especially meaningful over the long term. Because they replace the root as well as the crown of a tooth, implants protect the jawbone from the resorption that typically follows tooth loss. That bone preservation helps maintain facial contours and prevents the sunken appearance that sometimes accompanies long-term denture wear.
Implants are also designed for durability. With proper planning, placement, and ongoing oral hygiene, they can provide functional service for many years. Their secure fit eliminates common denture-related inconveniences like movement during eating or speaking, and implants do not develop cavities, making their long-term maintenance straightforward.
From a practical standpoint, implants can preserve the health of adjacent teeth. Unlike conventional bridges that require altering neighboring healthy teeth to act as anchors, implant restorations can often be completed without compromising adjacent tooth structure, which helps maintain overall oral health.
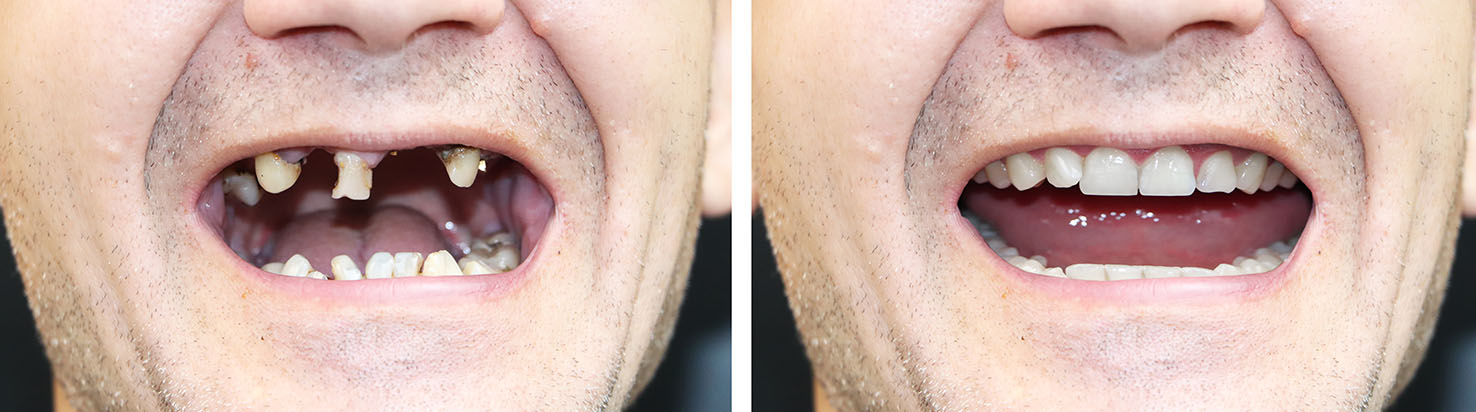
Implant restorations are not one-size-fits-all. Depending on how many teeth are missing, the condition of the jawbone, and your personal preferences, implants can be configured as single replacements, supports for multiple crowns, fixed full-arch bridges, or attachments for removable overdentures. Each configuration offers distinct advantages depending on functional and aesthetic goals.
Choosing the right approach begins with a thorough evaluation that includes dental imaging, oral health assessment, and a discussion of lifestyle considerations. This comprehensive view helps determine how many implants are needed, their ideal placement, and the type of final prosthesis that will deliver the best balance of comfort, function, and appearance.
Our goal is to match the appropriate solution to each patient’s unique needs, whether that means a single implant to replace one lost tooth or a strategic placement of several implants to support an entire arch of teeth.
Candidacy for implants depends on several factors, including overall health, oral hygiene, and the quality and quantity of jawbone at the proposed implant site. Many patients qualify for implant treatment; others benefit from preparatory procedures such as bone grafting or periodontal therapies to ensure a stable foundation.
During your consultation, we review your medical and dental history, perform a clinical exam, and obtain the imaging needed to assess bone structure. We’ll discuss any steps needed to prepare your mouth for implants and help you understand the sequence of care so you can make informed decisions about treatment.
Age alone is not a limiting factor — adults of many ages successfully receive implants — but each plan is individualized to address unique health considerations and desired outcomes.
Comprehensive treatment planning is the backbone of predictable implant care. We use advanced imaging and diagnostic tools to plan the exact location and angle of each implant, which improves surgical precision and the long-term success of the restoration. Surgical guides and digital workflows help translate the plan into accurate placement.
Implant placement is typically performed as an outpatient procedure. Depending on the complexity, it may be completed in a single stage or carried out in phases with appropriate healing intervals. Many patients receive a temporary restoration that allows them to function and maintain appearance while the implants integrate with the jawbone.
Follow-up care focuses on monitoring healing, ensuring proper integration, and eventually delivering the final prosthesis. Our team provides clear pre- and post-operative instructions and supports patients through each phase of recovery to promote predictable healing and comfort.
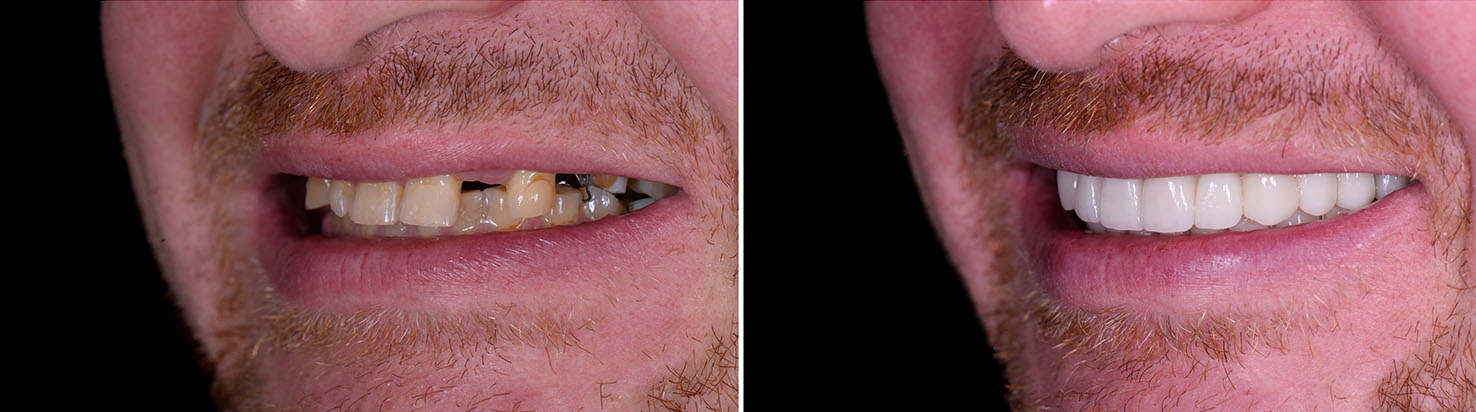
Sufficient bone volume is essential for the long-term stability of implants. If bone loss has occurred from periodontal disease, trauma, or long-term tooth absence, bone grafting can rebuild the foundation needed to support implants. Grafting materials and techniques vary, and the choice depends on the amount and location of bone needed.
Bone grafting is a well-established procedure that, when indicated, significantly expands the number of patients who can receive implants. The grafted area is allowed to heal and integrate before implant placement, providing a reliable base for osseointegration and the final restoration.
We’ll explain whether grafting is advised in your case and how it fits into the overall timeline so you can plan for each stage with confidence.
Replacing missing teeth with implants is an investment in your oral health, function, and self-confidence. The right restorative plan can preserve bone, protect adjacent teeth, and restore a reliable bite that supports everyday activities and a natural appearance. Our team emphasizes thoughtful planning and personalized care to achieve outcomes that last.
Village Dental of Leesburg is dedicated to guiding patients through each step of implant therapy with clear explanations and attentive follow-up. If you’re considering dental implants or would like to learn how they might apply to your situation, contact us to request more information or to schedule a consultation with our team.
A dental implant is a small, biocompatible post—usually titanium or a titanium alloy—that is placed in the jaw to replace a missing tooth root. Through a process called osseointegration, the bone bonds to the implant, creating a stable foundation for a crown, bridge, or denture. This root-like support restores mechanical function and helps distribute chewing forces to preserve bone.
By replacing both the root and the visible tooth, implants improve chewing, speech, and the long-term health of the jaw. Implant restorations are custom-designed to match adjacent teeth in color and shape, producing a natural appearance. Because implants are fixed and securely anchored, they avoid many of the fit and movement issues associated with removable prostheses, which helps patients eat comfortably and smile with confidence.
Implants are often preferred because they preserve jawbone by transmitting chewing forces into the bone, which reduces the bone loss that follows tooth extraction. They also protect adjacent teeth since implants usually do not require altering healthy neighboring tooth structure as traditional bridges do. Implants are resistant to decay and, with proper care, can provide very long-term function compared with many removable options.
Their fixed nature eliminates common denture inconveniences such as slipping or clicking during daily activities. From a practical standpoint, implants expand dietary options and can improve speech clarity, making everyday life easier. Maintenance centers on good oral hygiene and routine professional exams rather than frequent repairs or relines.
Good candidates for implants are adults with adequate general health, controlled chronic conditions, and healthy gums free of active infection. Sufficient jawbone volume is important for predictable placement, although many patients who lack bone can become candidates after preparatory procedures. Factors such as smoking, uncontrolled diabetes, or certain medications can affect healing and are considered during candidacy evaluation.
The initial evaluation includes a medical and dental history review, clinical examination, and radiographic imaging to assess bone quantity and anatomical risks. Based on those findings, the team discusses whether additional steps—like bone grafting or periodontal therapy—are recommended before implant placement. A personalized treatment plan outlines the sequence of care, expected timelines, and any alternatives so patients can make informed decisions.
Comprehensive treatment planning begins with 3D imaging and diagnostic records that allow precise mapping of implant positions relative to nerves, sinuses, and adjacent teeth. Digital planning often leads to the fabrication of a surgical guide that improves accuracy during placement and reduces intraoperative surprises. Placement is typically done as an outpatient procedure under local anesthesia, with sedation options available to reduce anxiety when appropriate.
At Village Dental of Leesburg, our team coordinates surgical and restorative phases so patients receive clear instructions, appropriate temporary solutions, and attentive follow-up care. After implant placement, a healing interval allows osseointegration and patients return for monitoring and adjustments to temporary restorations if needed. Once integration is confirmed, the final prosthesis is fabricated and seated, and the team reviews care steps to support long-term success.
The time from implant placement to delivery of the final restoration varies depending on implant stability, bone quality, and whether grafting was required. Some cases allow for immediate or early provisional restorations, while others follow a more traditional healing interval of several months to ensure predictable osseointegration. Complex full-arch reconstructions or staged approaches can extend the overall timeline, but each phase is planned to optimize outcomes.
Patients typically receive periodic checkups during healing so clinicians can confirm integration and make necessary adjustments to provisional appliances. When the implant is stable and the tissue has healed, impressions or digital scans are taken to design the final restoration for proper fit and esthetics. Final delivery includes occlusal adjustments and patient education on home care and routine maintenance to protect the investment in oral health.
Bone grafting is recommended when the jaw lacks sufficient height or width to support an implant with long-term stability, often due to prolonged tooth loss, periodontal disease, or trauma. Grafting materials range from the patient’s own bone to processed donor or synthetic materials, and the choice depends on the volume needed and anatomical location. In some cases, sinus lift procedures are used to create adequate bone in the upper jaw behind the molars.
After graft placement, a healing period allows the graft to integrate and be replaced by the patient’s own bone before implant placement is attempted. Careful surgical technique and appropriate post-operative instructions reduce complications and help ensure a solid foundation for later implants. Grafting expands the pool of patients eligible for implant therapy and contributes to more predictable, long-term results when indicated.
Single-tooth implants replace one missing tooth with an individual implant and crown, preserving adjacent teeth and delivering natural function. Implant-supported bridges use implants as anchors for multiple missing teeth in a row and avoid the need to alter healthy neighboring teeth. Full-arch fixed reconstructions can recreate an entire dental arch using a strategic number of implants to support a nonremovable prosthesis, while implant-retained overdentures snap onto implants to greatly improve stability over conventional dentures.
Each restorative format has distinct functional and maintenance considerations, so selection depends on the patient’s anatomy, hygiene capacity, and personal preferences. Treatment planning evaluates how forces will be distributed, how the prosthesis will be cleaned, and what esthetic outcomes are desired. A coordinated surgical and restorative plan ensures the chosen format performs reliably and fits comfortably within daily life, and your clinician will explain the pros and cons of each option during consultation.
Maintaining dental implants centers on meticulous daily oral hygiene, including brushing twice a day and cleaning around implant restorations with interdental brushes or floss designed for implants. Removing plaque biofilm at the gumline and between teeth prevents peri-implant inflammation and supports long-term stability. Regular professional cleanings and periodontal assessments allow clinicians to detect early signs of issues and address them promptly.
During the healing phase, patients are advised to follow the practice’s post-operative instructions, avoid smoking, and maintain a soft diet as recommended to protect the surgical site. Once fully restored, patients should continue periodontal maintenance and schedule periodic radiographs so bone levels and implant integrity can be monitored. If brushing or cleaning causes persistent redness, swelling, or discomfort, patients should contact their dental team for evaluation.
As with any surgical procedure, dental implant treatment carries potential risks such as infection, slow healing, nerve irritation, or sinus complications in the upper jaw, though these outcomes are uncommon with careful planning. Early detection and management are important, so clinicians monitor healing closely and advise patients on signs that warrant prompt attention. Smoking, uncontrolled systemic conditions, and poor oral hygiene increase the likelihood of complications and are important considerations during planning.
Minimizing complications involves thorough diagnostics, precise surgical technique, and adherence to pre- and post-operative instructions, including medications when prescribed. If problems arise, timely intervention such as professional cleaning, antibiotics, or corrective procedures can often resolve issues and protect surrounding structures. Long-term success depends on a partnership between the patient and the dental team to maintain oral health and respond quickly to changes.
When choosing a provider for implant treatment, consider the clinician’s training, surgical experience, and the restorative dentist’s ability to design esthetic, functional prostheses. Look for a practice that uses modern diagnostic tools such as 3D imaging and digital planning to enhance precision and reduce surprises. A coordinated team approach that includes implant surgery and prosthetic planning improves the predictability of outcomes, and clear communication about the treatment sequence, risks, and expected timelines is essential.
Village Dental of Leesburg combines experienced clinicians, digital workflows, and a patient-centered process to guide candidates through planning, surgery, and restoration with attentive follow-up care. During an initial consultation, ask about the practice’s typical treatment protocols, available sedation options, and how they monitor healing and long-term maintenance. Choosing a provider who prioritizes safety, clear explanations, and individualized planning helps ensure a smoother experience and reliable results.
